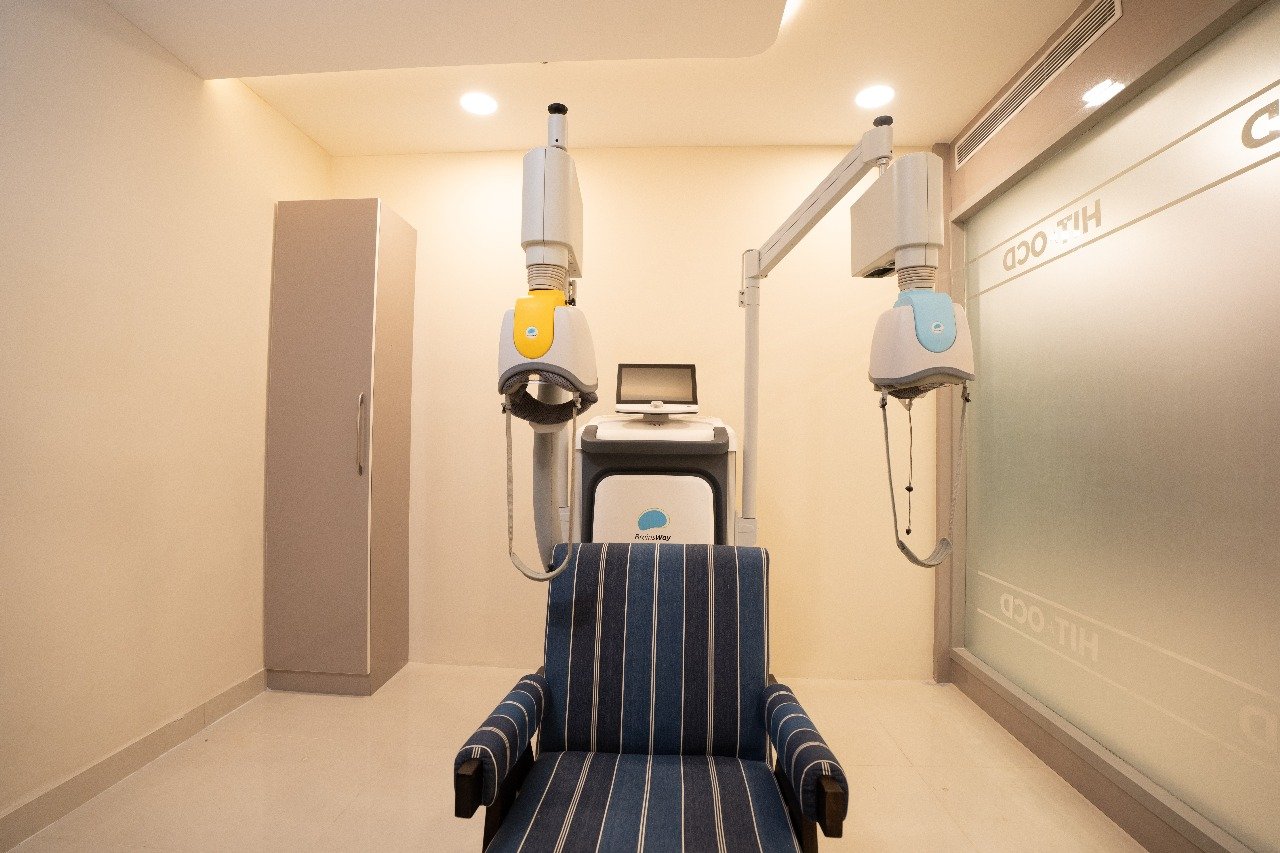
HIT with PET
HIT-OCD, or High Intensity Treatment for OCD, is an intensive outpatient program designed to enable faster, functional recovery for patients. The hallmark of HIT is PET – the combination of Pharmacotherapy, ERP, and TMS, three highly effective, evidence-based treatment practices
Pharmacotherapy
Pharmacotherapy, or the use of pharmacological drugs, is a widely accepted first-line treatment for OCD. The most commonly prescribed form of medication are SSRIs, of which specific medicines are selected according to the needs of the patient.
ERP
ERP, or Exposure and Response Prevention Therapy, is a gold-standard therapy for the treatment of OCD. A form of Cognitive Behaviour Therapy, it places emphasis on exposure to OCD-related triggers and the learning of coping techniques to deal with the resulting anxiety. Over time, individuals develop resistance to their obsessive thoughts and urges, in a process called “habituation”.
Transcranial Magnetic Stimulation
Deep TMS (DTMS) is a treatment approved by the US FDA in 2018 for its application in OCD treatment. The H7 coil by Brainsway is designed to stimulate the MPFC and ACC, two brain areas associated with the development of OCD. When used alongside medication and therapy, DTMS has been found to be safe and highly effective for treating OCD, with faster recovery times.
Holistic Healing
Along with the PET treatment program, HIT offers holistic therapeutic approaches such as Individual, Group, Family Counselling, Art, Music Therapy and Yoga.
Continued Therapy
In addition to five days of intensive outpatient treatment, HIT-OCD includes a maintenance period of six months, during which patients build on their initial progress. Patients are given maintenance DTMS sessions, their medication is monitored, and they are provided additional support from psychiatrists and psychologists as needed.
Opening Doors for Self-Recovery
While HIT-OCD cannot guarantee an OCD-free life post treatment, the program sets patients up for success, with tools and techniques to manage their triggers and compulsions. HIT helps patients reclaim their time and energy for activities and goals that bring them joy and purpose.